One of the best ways to heal yourself and to help heal others is to share! If you are a fighter, survivor, caregiver or a medical professional and you have a story of courage, bravery or triumph, I would love to hear from you! Please email me your story, along with a picture of yourself or one relevant to your journey (if you’d like one posted) at Michelle_Burleigh@Hotmail.com or by clicking Contact in the above menu.
I will do my best to post all stories within 1 week.
Disclaimer: I’m looking to keep this site clean. No detail is too detailed here but please keep the language tasteful. Thanks!
(DUE TO COVID19), THE PARAMEDICS TOLD ME IT’S JUST TOO RISKY TO GO TO THE HOSPITAL
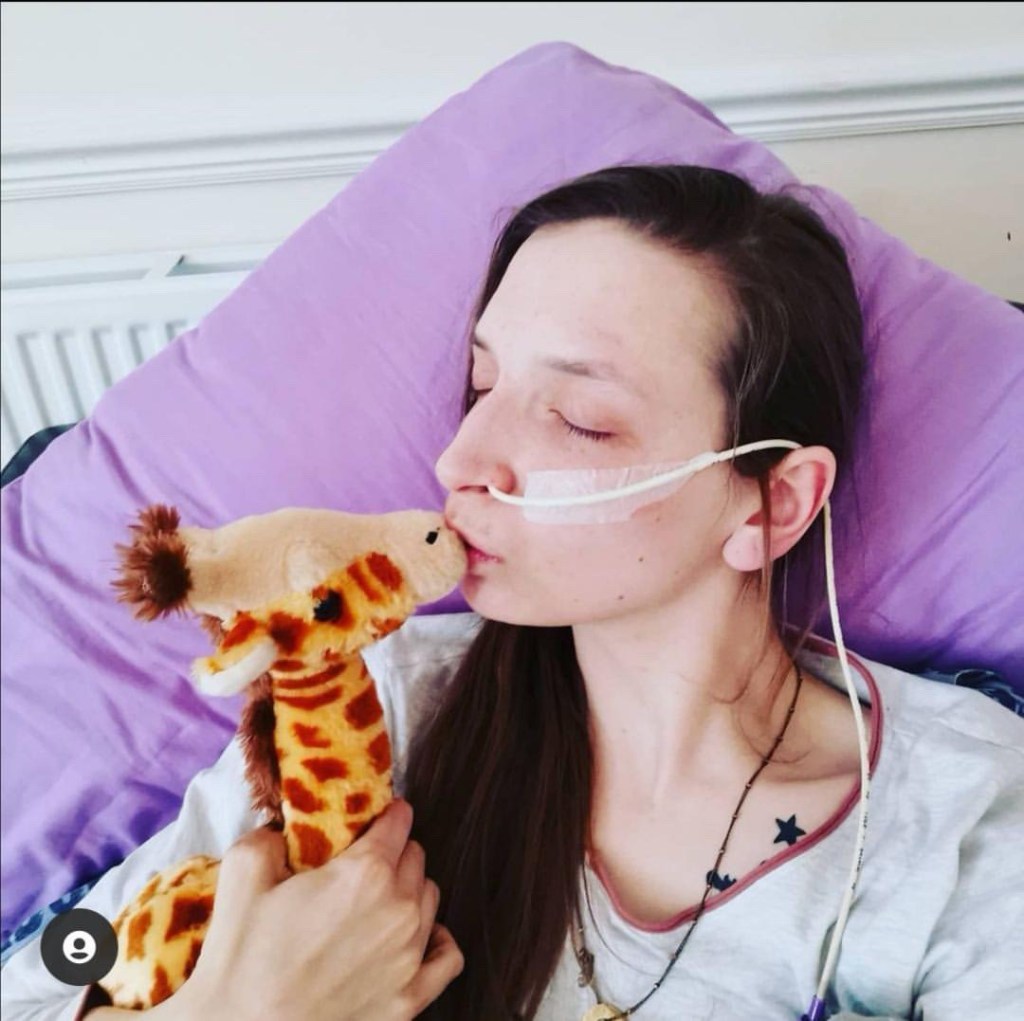
fEBRUARY 13, 2021 – SO YOU’VE GOT CANCER…JOIN THE CLUB!!!
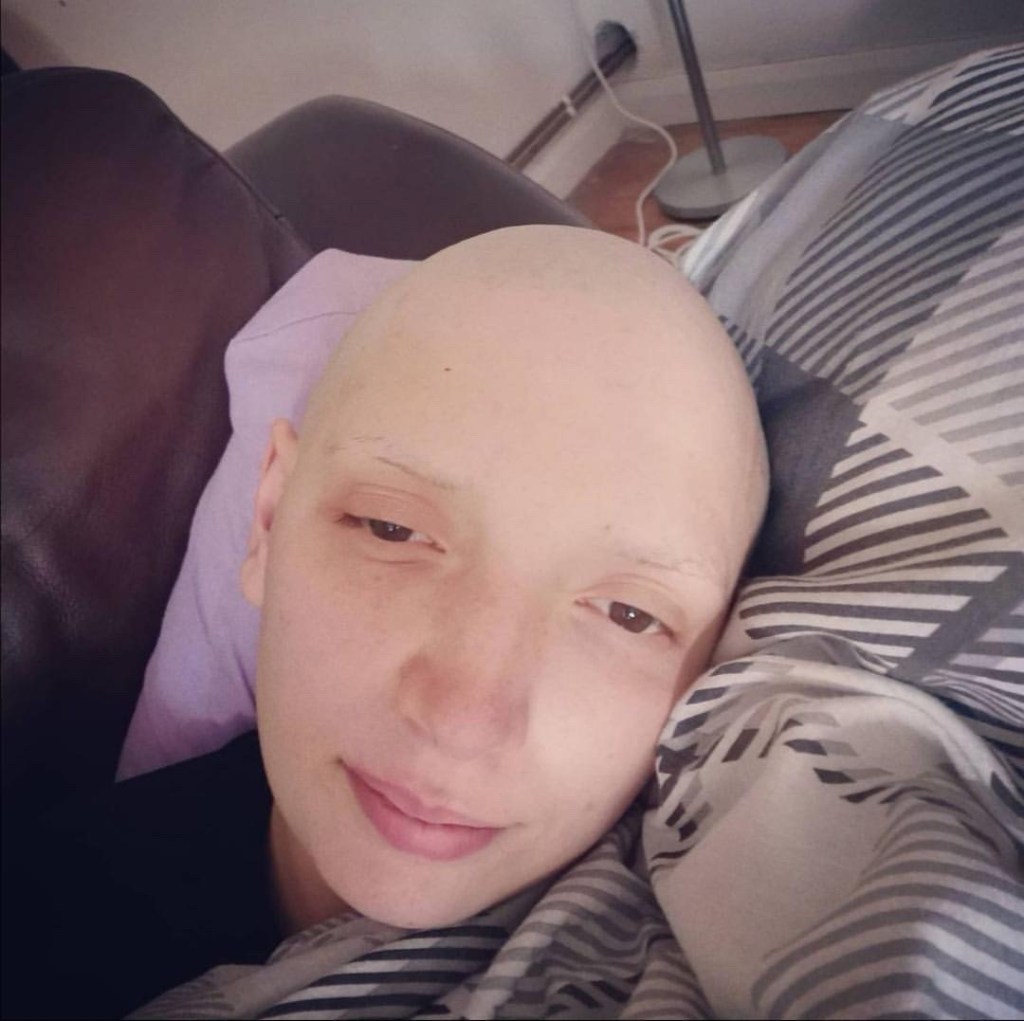
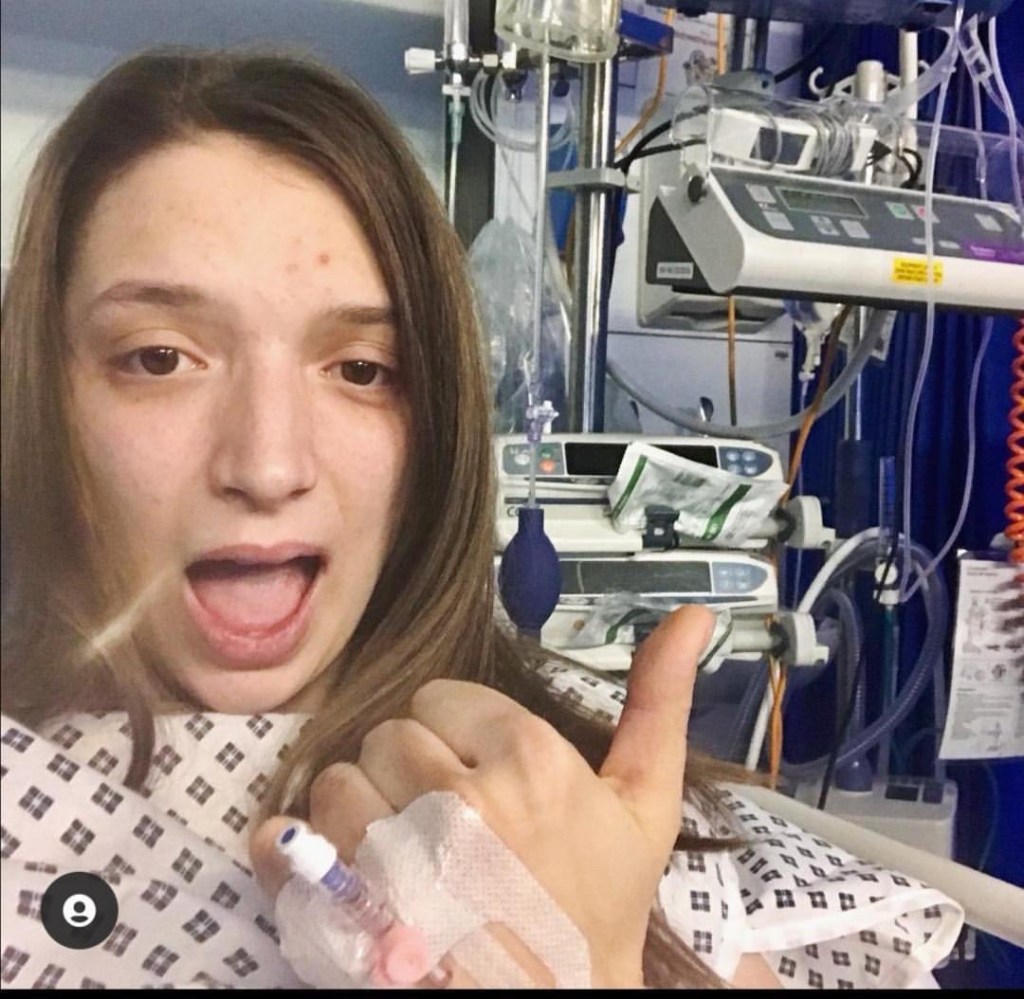
BY: HATTY FREEMAN (@SURVIVINGHATS ON IG)
One night I sat on the sofa and suddenly I had an excruciating pain in my stomach. I was 14 years old so my parents rushed me to hospital and they immediately, in a panic, diagnosed me with appendicitis. I was into surgery within the hour. When I woke up my blood test results had come back and they realised that my blood counts were very very wrong. My white blood cell count was very low as well as other things. When they studied my appendix they found leukemic cells and realised that my pain was coming from cancer cells building up within my organs. I was in a small town hospital so they moved me to a bigger hospital in the city of Oxford (England). There they did a bone marrow biopsy which confirmed acute promyelocytic leukaemia. This is a rare sub type of acute myeloid leukaemia and was thought very treatable, also very fast acting so they needed to treat me quickly. They put me on a drug called ATRA, the simplest way to explain this drug is that it’s a toxic dose of vitamin A and it’s taken in a pill 1 pill a day and is not particularly pleasant. They also started me on arsenic trioxide infusions once a day for 50 days (I know this sounds awful, but it’s a very effective treatment). I was also started on idarubicin which is a chemotherapy drug, this drug made me very very sick.
I stayed in hospital for that time. I was a high risk patient because my white blood cell count was so low. After this ordeal I did go into remission. Sadly this remission only lasted about two months. They did the same cycle of treatment again adding a slightly higher dose of idarubicin. This did put me into remission, however there was still leukemic cells in my spine and my lungs, so they added in some radiation. I relapsed a third time about two years later by this time I needed chemotherapy into my spine as a lumbar puncture, my lungs were severely compromised and I began to have breathing problems. They put me on high dose Cytarabine which is kind of a last resort for this type of leukaemia however by some miracle it did work and though I didn’t get into complete remission I was well enough to continue with my life and learn to live with cancer.
What I would call my 4th relapse was when we decided to start trying clinical trials. The drugs, of which I can’t spell or pronounce so I won’t even bother, were very very rough. They were given to me just before the pandemic so when we were having issues with my breathing the paramedics would turn up and say it’s a high risk for me to be going into hospital, and that it is probably better for me to stay at home. So, they gave me the drugs I needed to get my breathing back to normal and then left me at home. I was having seizures, multiple seizures everyday. It was a terrible time. I was screaming in pain but nobody knew how to help me, and by nobody I mean my housemate. Because of COVID-19 we where completely alone. It was a real lack of help due to the situation and, honestly, the last place I wanted to be with in hospital because I knew how risky it was (to be there). If I were diagnosed with COVID-19, I would probably be toast.
Now I’ve just had high dose Cytarabine alongside another trial drug which again I cannot remember the name. I’m in a lot of pain. Luckily, I’ve met a lot of beautiful people online who have kept me going through this entire journey and I have a wonderful group of friends and, now we’re in lockdown again, I’m very lucky to have such a wonderful housemate who looks after me whenever I need it. I am very tired at this point after 12 years of fighting. I’m now 26 and I know that I’m very lucky to have gotten this far so I should be celebrating, and I am. I’m very very grateful. I’m mostly grateful for the people around me who have kept me going through the highs and lows a cancer diagnosis bring and I love them so much.
WHEN I MET THE CONSULTANT AND HAD ‘THE TALK’, I WAS PETRIFIED – IT SOUNDED LIKE A GAME OF RUSSIAN ROULETTE

JANUARY 28, 2021 – SO YOU’VE GOT CANCER…JOIN THE CLUB!!!
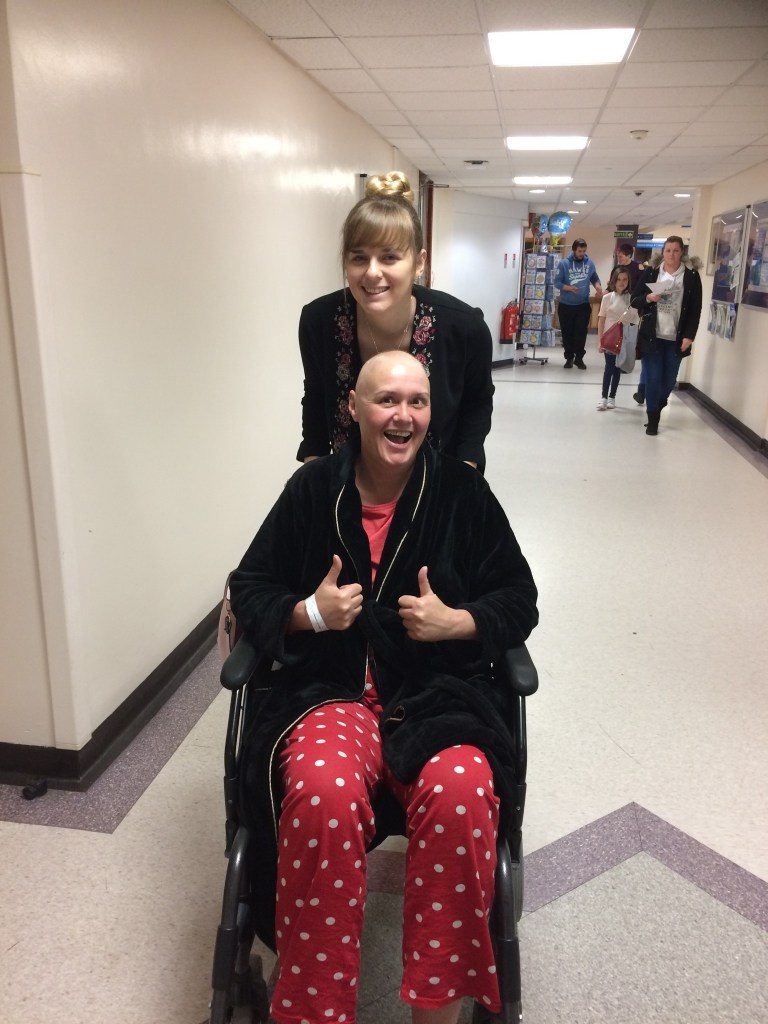
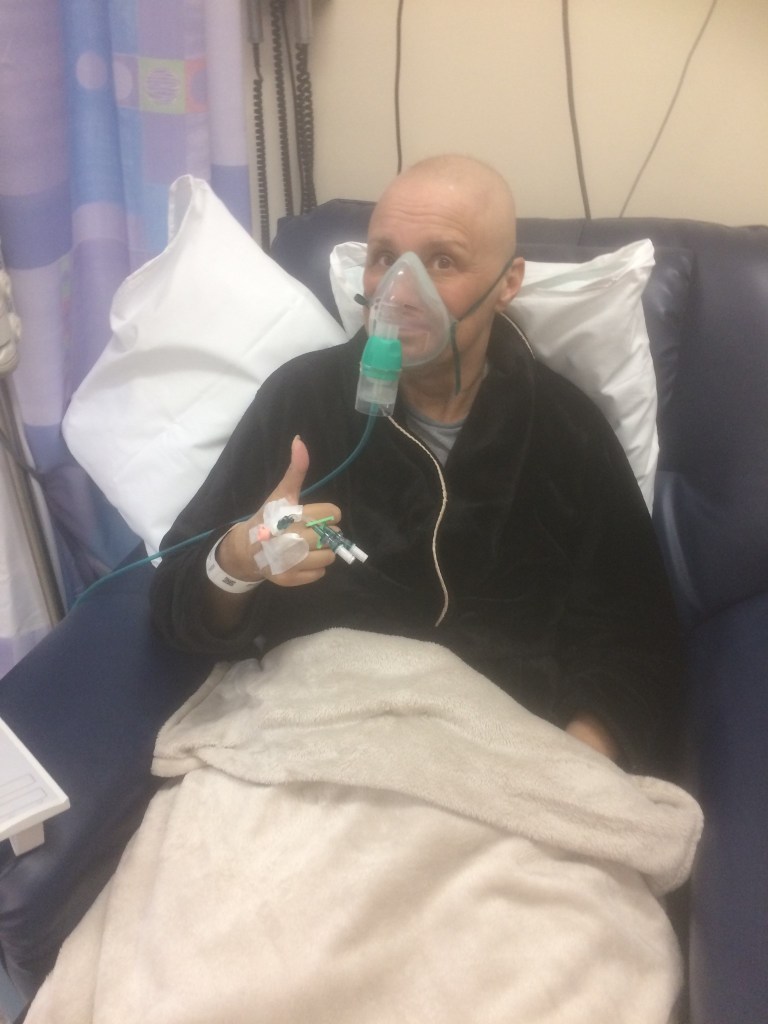
BY: TRACY RICHARDSON (tracyrichardson1@sky.com)
I’d been unwell on and off for a year or more and can’t really say this was related, but more symptoms started to appear over the course of a few months. I started having dizzy spells, aching joints, bruises, tiredness and a persistent nosebleed. I also had what I thought was a chest infection which turned out to be pneumonia.
My initial diagnosis consisted of the following:
- Grief from the death of my Father
- Depression
- Perimenopause
- Knee joints not connecting properly
- 6-hour nosebleed wasn’t diagnosed as anything
It took five visits to the doctor and a trip to Accident & Emergency before I was offered a blood test.
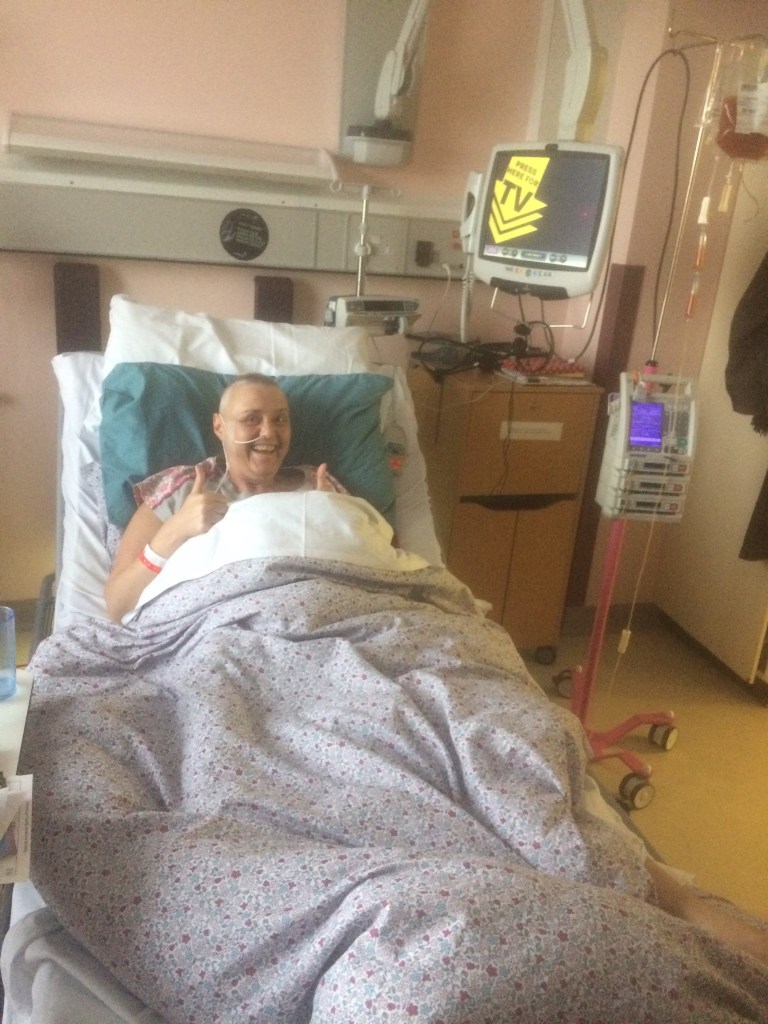
After having a blood test, I got the call from my doctor on 29th September 2017—my partner’s birthday—that shook me to the core and completely turned my life upside down. The blood tests showed I had acute myeloid leukaemia (AML). I was told to pack a bag immediately and head straight to hospital. There I met my consultant, who took my bloods to confirm exactly what type of leukaemia I had, and told me I had 80% blasts and maximum 12 days left if I didn’t agree to chemotherapy almost straightaway. My family were all informed and were devastated, as was I.
Little did I know that this was to be my home for the next six weeks.
I started my first round of chemo and likened it to cherryade as it was bright red. This knocked me for six and I developed a rash all over my body. I also had mucositis, a painful mouth infection where my gums ended up covering my entire teeth and I had numerous ulcers. For two weeks I lived on soup, ice cream and mash. I’d never felt so ill in all my life and the fatigue was indescribable. I became bed bound. My hair was falling out so my friend came to the ward and shaved my head as I would find my hair everywhere. I donated my hair to the Little Princess Trust as it was very long.
Results from bloods and the dreaded bone marrow biopsy I had to have revealed that the chemo hadn’t put me in remission and the blasts were still there. It was now becoming a race against time, so after a short break at home to recuperate, I was admitted for the next round of chemo. This time it was going to be more potent and toxic. I likened this one to Irn-Bru. My fighting spirit came out for this round and, feeling stronger this time than the first, I was determined to get better and beat it.
After my next biopsy, it showed I was in remission and I was elated, but this was short lived because the results also showed that my bone marrow had taken a battering, giving me grade 4 fibrosis. This meant it was extremely likely the leukaemia would be back within months and with a vengeance, so the only possible solution would be a stem cell transplant.
I was scared as I knew little about what this entailed, but it sounded like my only choice. A meeting was set up at a hospital 75 miles away from home, and when I first met the consultant and had “the talk”, I was petrified—it sounded like a game of Russian roulette; it might work and it might not. So many side effects and talk of death made me realize I had a massive decision to make and I wasn’t sure if I was strong enough or my body could take it. Many nights were spent crying. I decided to go ahead and try to save my life in any way I could, regardless of the worst-case scenario.
First, I needed a donor. My brother and sister weren’t a match, so Anthony Nolan (a stem cell/bone marrow registry – click here for more info) were contacted and they amazingly found me a 10/10 match with a 30-year-old male from North America. I was over the moon and so very grateful for this selfless person who would donate their cells for me. The date was set for my transplant and the hospital was to be my home for the next few weeks. Fortunately, my partner was able to stay on the grounds.
I was given a sheet with my regimen on for intensive conditioning therapy and antibodies, and this treatment was going to be one of the hardest parts to get through, as I knew from “the talk” that the side effects could be extremely debilitating, as could the fatigue. After getting through the regimen, my transplant date was 8th February 2018 which was to become my re-birthday.
It was an incredibly emotional time watching my donor’s cells infused into me and giving me a second chance at life.
I was in hospital for three weeks, and as soon as my neutrophils reached 0.5, I was allowed home. I was still classed as neutropenic and had to be careful with what foods to avoid. Plus, a list of things to be careful with and rules to follow. The overwhelming tiredness and fatigue and being wheelchair-bound made me realize just how much my body had been through. Not to mention the emotional impact of it all. The side effects had been pretty gruesome, especially the BK virus where I was on the loo every 20 minutes, but with a determination and strength and love and support from my family I had come out the other side.
Those first few months were spent mainly indoors as I had no immune system, and if I did venture out, I had to wear a mask for protection. I had to take 35 tablets a day and I’m no tablet taker. Clinic appointments were twice a week with regular blood checks, and a bone marrow biopsy showed I had 100% chimerism meaning I’d completely harvested my donor’s cells and was now 100% donor. This was the best news I could have wished for.
I was borderline 100 days when I developed GvHD (Graft-versus-Host-Disease) of the gut, showing bowel and gut problems. I was admitted and ended up being on the ward for a month. I was put on prednisone steroid tablets and whilst they helped my GvHD, they brought on a new set of challenges over time.
After taking steroids I started gaining lots of fluid in my legs, and at one point my knees were measured and they were 52cm. This left me virtually immobile as my legs were so heavy and I was covered in blisters that oozed fluid, making me leave puddles wherever I had sat. Emotionally this was another particular low point. District nurses told me not to worry, but when I developed an open sore on my foot, I knew this was serious. I got admitted and the consultant told me that my protein was dangerously low and it didn’t look good. I also had a foot ulcer and was close to losing my foot. I found myself having to fight for my life yet again. I was on the ward for two months and within that time I became steroid-induced diabetic and caught numerous infections, something else to contend with, but I was alive and that was all that mattered.
After two months I was transferred to my local hospital and spent another month recuperating and having physio as I was still immobile and had lost all my muscle mass. Over time I beat diabetes and came off steroids and my protein returned to normal, so I was allowed home.
I’m 21 months post-transplant and still in remission, something I never thought I’d be in those early days of diagnosis. I have thanked my donor for saving my life and hope to meet or correspond one day. I do live with side effects from the chemo and transplant, but it’s a small price to pay for living. Slowly but surely my mobility is returning. On a bad day I still use a wheelchair for long distance and on a good day I walk with a stick. Not bad for saying I very nearly lost a foot and couldn’t walk at all.
I’m always being told I look well but it’s very hard for those that haven’t gone through my journey to understand lasting side effects. I have since been diagnosed with PTSD and am only just being referred for CBT and counselling. I don’t feel there is enough out there to cater for the emotional impact of leukaemia as it’s such a long journey, with lengthy hospital stays and readjusting after being extremely hard I have found.
I hope my story will help raise awareness of the symptoms that are all too commonly shrugged off by doctors, and will help people recognise what the symptoms are.
[THE DOCTOR] ASKED ME IF I HAD BEEN SHORT OF BREATH, OR TIRED LATELY. I TOLD HIM, ‘I WORK, GO TO SCHOOL AND I AM A MOM, OF COURSE I’M TIRED’.
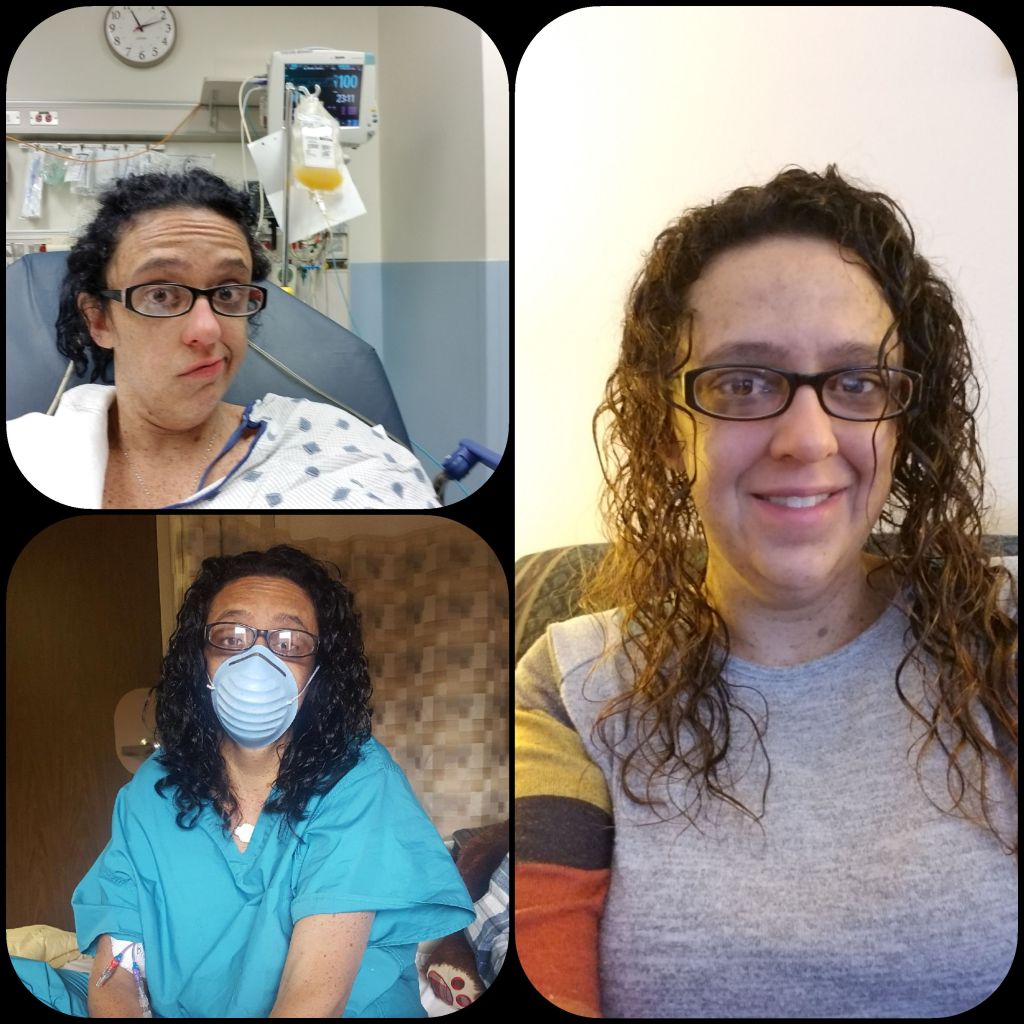
January 22, 2019 – So You’ve Got Cancer…Join the Club!!!
BY: SHAWNA JOHNSON
Mother’s Day 2018, my world was turned upside down. I was 30 years old and had just finished my first semester of Nursing school. My fiancé, kids and I were home, putting together the bike my son got for his birthday. He was going to be at his dad’s house for his birthday so we decided to give him his bike early so he could ride it. We had spent the day at a soccer game, then a graduation party for my friend who just graduated the nursing program. My nose had been bleeding off and on for two days. As I was leaning over to help put the bike together blood would drip, I just couldn’t get it to stop. After a phone call to my Primary Care Provider (PCP), I was directed to the emergency department (ED) to get my nose cauterized. I decided I better go. I said goodbye to my family and took the 40 min drive to the hospital.
I was fairly irritated that I was going to the hospital and that my nose just wouldn’t stop bleeding. I called a friend on the way to the hospital to tell her I was going in, we batted around the idea of going to urgent care instead of the ED, I even called urgent care to see if they were able to cauterize my nose. I eventually decided to just go to the ED. I walked in, feeling foolish with this bloody nose and there were other people around who needed help. I was given one of those clips to put on my nose and told to sit down and wait to be called. I sat there with this annoying clip on my nose for 15 minutes before I was called.
A triage nurse took my vitals, and as I told my story one of the ED doctors over heard me. He came out to talk to me, he asked if I had any thing else going on. I mentioned I had some weird bruising. We have a pet pig who lives in our house, he was little and liked to lay on my lap. I had some bruises on my inner thigh, I also had a big one on my outer thigh from when I ran into a desk at school. There was also one on my back from a back massager I was using while studying for finals. I was just full of them. I bruise extremely easily and always have, so to me, these were nothing. He asked me how long I had them for and I said a couple weeks. He immediately said he was going to draw some labs. This was nothing alarming for me, I have lupus and get my blood drawn from time to time. He sent me back to wait to be brought to the ED, I waited and felt bad, all I had was a bloody nose. There were other people in the waiting area, coughing, crying children and then me. I thought to myself I am going to take up the doctors’ time when there are people who need them more.
I was finally called back into the ED. I sat on the bed as the nurse ask me why I was there, I explained myself all over again and she said, “ok change into this gown and the Doctor will be in shortly”. As I sat there for what seemed like forever, I finally over heard my name being mentioned. I couldn’t hear what else was being said and shortly there after a doctor walked in. He asked me if I had been short of breath, or tired lately. I told him “I work, go to school and I am a mom, of course I am tired”. He didn’t smile, he sat there for a moment and then told me what my CBC came back as. Yes, I am in nursing school, but I just could not tell at that moment whether those numbers were in range or what. He asked if I had ever had a blood transfusion, “Umm no?”, he said I am going to give you some platelets and make a phone call. I was so confused, my fiancé was home with the kids, and I had nobody with me.
I called my mom and texted a few friends. I sat there as the nurse came in and attempted to place IV. That did not go well. Finally, after a second nurse came in, they were able to place the IV. The nurse asked me the questions needed for blood transfusions and went over the side effects and when to call, if needed. The last chapters in class were about blood transfusions so I was very aware of when to call. Platelets went in with no problem. I figured I was able to go home; the beeping of the infusion pump was quite annoying, and I was ready for bed at this point. The doctor came back in and told me he was admitting me, and I was sent to the neurology floor.
The neurology floor is when things became confusing and blurry. I was put on so many medications right away and I became sick and hardly able to stay awake. Everything that I ate came right back up. Everything I did from looking at my cell phone, to just sitting up made me vomit. Then I received the news, “You have leukemia”. I don’t even fully remember being told. I remember being told I need to start on ATRA right away and need a bone marrow aspiration in order to confirm the type of leukemia. The aspiration was done the next day, on Monday. Then I was moved to the oncology floor.
The results came on Wednesday, “You have Acute Promyelocytic Leukemia”. This time I remember these words. My mom had driven from her home in Illinois to my hospital in northern Minnesota. We cried as the Doctor told us the news and explained this leukemia to us. My son was the first person to cross my mind. He was 4 years old, turning 5 in a few days. I was so afraid that I was dying, the doctor told me that out of all the leukemias out there, this was the one to get. He said the cure rate is 98%, and we will be starting the 85 days of Arsenic Trioxide treatment right away. He said I would be in the hospital for up to 85 days and I needed to be closely monitored for differential syndrome. This can be a fatal part of APL with fevers, respiratory distress and other factors.
Slowly I became acclimated to the oncology floor. I made friends with my nurses and had visitors most days I was there. My fiancé came every day and brought my step-son, my ex brought my son most days and even stayed a few Saturdays for many hours so that my son and I could be together. My mom was there for the first two weeks, my dad was there with me for another week and a half, plus all my amazing friends that were there to support me. My fiancé threw me a party in the lounge with my friends and mom, for my 31st birthday. My aunt and cousin came from Arizona for a few days as well.
Treatment side effects were fairly awful, but the treatment was saving my life. I experienced horrific headaches and dry lips from the ATRA, my lips cracked so bad they would bleed. The arsenic caused swelling in my feet and legs-my friend called me sausage feet (it was so funny), and my liver enzymes went through the roof causing treatment to be stopped for a week in the middle of it. My day consisted of blood draws, EKG’s, 3 hours of treatment, blood transfusions along with cryoprecipitate (clotting agent) and trying to keep myself busy. I received so many transfusions I lost count. I walked the halls, colored adult coloring books and taped the pictures to my walls (the nurses and doctors sure got a kick out of the colorful words and sayings on my walls), played games with visitors, watched movies, and napped.
I remember my oncologist coming in to see me one day and I was napping. He came in a few days in a row and I happened to be napping each day. I woke up at 4am usually due to the ATRA headaches so naps were normal for me. He came in and said to me that I needed to get up and get moving, he gestured at me that people die like this (laying down), people live like this (standing up), I think he thought I was depressed and never did anything with my day. One day my legs started to hurt, I thought it was muscle aches from keeping my legs up all day, again my legs and feet were so swollen I could hardly walk, I had compression socks on all day and feet up all day and was on Lasix to help get rid of all the fluid. The cramps were in my hip joints, my groin area. Oh, did it hurt, it got so bad that one night I called my nurse crying and said, “ok something is wrong”. They had given me flexural (a muscle relaxer) prior to this and it was unbearable. He immediately called the doctor who sent me for a STAT ultra sound. The ultra sound told me to stay still while she did the exam, my legs and hips hurt so bad I was crying to entire time trying to stay still. Luckily the ultra sound was clean, no blood clots in my legs. I returned to the floor and my nurse had orders for another lab draw. Sure enough, that lab draw came back with sky rocketed white blood cells. Which was what was causing the pain, I was put on a new medication to lower the white blood cells. The medication took about a week or so to fully work, my legs hurt so bad during that week, getting on and off the toilet or a chair was a chore. Being on Lasix which makes you have to pee a lot and having that pain, was not a fun week.
The visitors helped so much, and I was in constant communication with the ones that mean so much to me and helped me through. My blood counts eventually started to stabilize, and my numbers began to increase all on their own without the help of a transfusion. Then the day came, well night as my Doctor came in to my room at 8pm one night. He said those magical words, “you can go home tomorrow”, I happened to be on the phone with my mom who had returned home. I cried and asked him probably 4 times if he was sure, he said “yes, tomorrow you can go home.” I still had to come back every day for treatment, lab draws and EKG’s. I had a port put in the day I was to go home, which delayed me leaving the hospital a little bit, but I was still able to go.
32 days in the hospital-32 long days away from home, and I was finally free to go home. I walked out of those hospital doors and cried most of the way home. The smells of everything around me just made me so happy. The fresh air, the smell of the freshly cut grass, even the paper mill, which, let me say, does not smell nice at all, but it was a familiar smell from my hometown.
Home at last! It was amazing to be home, with my family and able to sleep in my own bed. Yikes, the stairs in my house were so difficult to climb. We don’t have too many but after not using them for a month I lost muscle tone. I highly recommend to anyone who has to stay in the hospital for a length of time, please talk to the physical therapy people and see if they will get you some work out bands. Home was great; however, I was afraid of everything. Being sheltered in the hospital with everyone washing their hands, clean sheets every day, no outside germs of any sort to come home to living on a farm with chickens, dogs, cats, and a pet pig was a bit drastic for me.
I was paranoid about every little germ and getting sick. I returned for treatment to the hospital for 3 days, the plus side was that my treatment got expedited from 3-hour infusion, to a 2-hour infusion so that was nice. Monday came and I was back in the infusion center, my oncologist found me there to tell me the results of my bone marrow biopsy. Remission. I had no leukemic cells in my bone marrow, I was off treatment for 2 weeks and then would begin consolidation. The two weeks off everything was great, I felt like things had normalized and just like that I was back at the infusion center for the now normal; blood draws, EKG’s, and infusion. The port was finally healed up and I was able to use it. I love my port, it made life just seem more normal. I did not leave my needle in as they suggested at first because the bandages made my skin raw and the needle just hurt. So, I chose to get accessed every day, with the lidocaine cream they gave me it was not a problem, I was unable to feel the needle being put in.
Cycle 1 came and went with not much excitement, which I was happy about. I had 4 weeks off treatment, I went back to work and was able to spend time with my family. Cycle 2 was fast approaching, and I was so nervous, I had an emotional breakdown. I cried for days before cycle 2 started, I told my oncologist I was so scared, he told me I had no reason to be worried, the treatment worked, and I no longer had leukemia, I was in remission. Cycle 2 started, and the nausea and headaches really got to me the first week, after that I was able to drink enough water, and eat enough junk food (I ate so much junk food) that I didn’t feel that awful. I decided not to feel bad about eating junk food, I was fighting still every day and if the junk food made me feel better and able to handle the treatment then I was going to eat it.
Cycle 2 finished and another 4 weeks off treatment. I had another conversation with my oncologist about going back to school, and he said there was no reason I couldn’t go as long as I was able to still come to treatment. I was super lucky enough to have all my classes start at 1pm so I worked it out with my scheduler to help me get into infusion as early as possible so with the labs and EKG’s I was still able to make it to class on time. I spoke to my instructors prior to classes starting and they were all understanding of my situation and knew that if I was late to class there was a reason behind it. Cycle 3 came the same week school started, I was so tired and felt incredibly nauseated the first week. My class on Fridays was 4 hours long and it was such a long day. I was exhausted by the first weekend of classes I didn’t want to do anything except sleep. The next week I talked to my nurses about the nausea, I chose not to take the Zofran they offered me because I had learned it prolonged my QT interval which is what they were watching on the EKG to make sure my “heart was not mad”. That is how I always put it, I was able to feel my heart beating when my magnesium and my potassium were not quite high enough, or my QT interval was getting too long. It was sort of strange, but I began to understand it more. One of my nurses suggested an anti-nausea medication that was IV and lasted 3 days, I was all about that! Yes please! I have class to get through and I just didn’t want to puke on anyone. Well, turns out I should have just gone through class being nauseated because I had an anaphylaxis allergic reaction to the medication. I began to feel short of breath and my chest got tight. Luckily my nurse was not too far away and I told her something was wrong. She stopped the infusion and got the pharmacist. They gave me some steroids and some Benadryl to stop the reaction and watched me for a little while. We decided I was not a candidate for that anti-nausea medication, and I chose to just deal with the nausea after that.
I made it through cycle 3 even with clinicals, I went to clinicals then went to infusion one day I was there until almost 5pm. That made for some very long days. Cycle 4, my last cycle finally was here! Oh, but it started on finals week! Finals week of my second semester of nursing school. I thought about asking if I could postpone treatment, just a week so I could take finals without feeling fuzzy and nauseated, but that would mean that I had one week of treatment during the first week of third semester, which third semester schedule was not nearly as nice as second semester, so that would mean I would be missing a class. So, I just chose to keep my original schedule and do cycle 4, week 1 and finals at the same time.
My first final was Tuesday morning and it was a computerized test, I made it through the test without puking on anyone which I thought was a great accomplishment. I passed my exam and I was beyond grateful! I still had one more to go, this one was written, cumulative and I was very nervous for this one. I studied during infusion and went to bed early, mostly because I didn’t feel well. I had infusion before my test that day and studied again. I took my test and anxiously awaited that text message that told me my grade. I was picking up groceries and got the text message saying I passed my final! I cried in the middle of the grocery store. I had officially passed my second semester of nursing school! I did this WHILE on treatment for APL! I felt like I concurred the world! I could not express how excited I was! I was so excited to tell my infusion nurses who were there for me and helped me work through things I did not understand. I also told my oncologist. I was just beyond excited. Cycle 4 came to an end and it was so surreal. My life was about to change again. 1 week into 2019 and I was done with treatment officially. The road seemed like it would never end, the repetitiveness of the last 6 months was just engrained into my head.
I learned so much about myself during this very traumatic time. Always take time for the little things. Never give up. Never let anything stop you for doing what you believe you can do. Don’t spend time worrying about what others think, spend your time with your family and friends making memories because in the end, they are the only ones who will be there for you.
I WILL NEVER FORGET THE PIT IN MY STOMACH WHEN HE SHOWED ME THE BRUISES

January 15, 2019 – So You’ve Got Acute Blood Cancer…Join the Club!!!
BY: LINDA PERRY
After a verydifficult year caring for my husband following a traumatic accident, lifestarted to finally feel somewhat “normal”. “A new normal, but nonetheless “normal” for our family. What an amazingfeeling, finally all being under the same roof after 4 long months.
A nurse byprofession, I took some time off to care for my husband following his accident.While caring for him, I questioned ever wanting to do nursing again. I had justbeen through too much. I needed happiness and positivity in my life andalthough caring for patients is rewarding in and of itself, I just feltdifferent about nursing now. The smells, the sounds of beeping machines,everything about it just felt different. After several surgeries and months ofrehab, I finally felt ready emotionally and physically to return to work.Ironically, while on leave caring for my husband, I was introduced by a friendto a woman who was in need of a companion for her ailing mother. I happilyaccepted the position and was scheduled to start July 6th.
In June2018, my husband complained of cough and congestion, and fatigue for a week orso which I initially attributed to simply a summer virus, and/or allergies andI began treating his symptoms at home with over the counter treatments whichlater proved ineffective.
It was notunusual for my husband to show up for work being as sick as he was, he has donethis many times before. Overtime had become scarce recently making it even moreimperative to show up during the busiest holiday of the year. The beaches werepacked due to extremely high temperatures predicted that weekend. Sick as he was,he was off to work from sun up to sun down beginning July 3 through the 5th.
Despite the best nursing scare tactics I could not get him to go to his primary care provider (PCP), or local ER for more immediate evaluation despite worsening of his symptoms including cough, shortness of breath with ANY exertion, and now excessive unexplained bruising.
On July 6th, he finally agreed to go to his PCP, but of course not until he did a few things around the yard. As he climbed into the woods in our backyard to grab our golden retrievers leash, he lost his footing and thankfully saved himself from completely falling by wrapping both arms around the tree in a hugging fashion. Feeling lousy, he finished up what he was doing in the yard and headed for a nice warm shower. I will never forget the pit in my stomach when he showed me the bruises covering over 3/4 of his arms less than a half an hour following his near fall. I knew in my heart something was terribly wrong.
He insistedon going to urgent care alone, assuring me he would be fine. “I probably havelow iron” he said, and off he went. I kept in contact with him during his appointment,and as expected they did lab work, vitals , etc. His oxygen saturation was at94% which was yet another red flag in retrospect. The last text message Ireceived from him said “they are sending me down to CT as a priority, they sawsomething on my lungs”. “Pneumonia?” Iasked, to which he responded “no, they saw something on my lymph nodes.” Not long after, he was brought back into theexam room, where he was given a preliminary diagnosis of Leukemia requiringimmediate admission to the hospital for further work up.
He called meto let me know of their concerns. I immediately became angry and upsetwondering why they would tell a patient “We believe you have leukemia” withouthaving all of the information to support this kind of diagnosis, “This is crazy”,so I thought.
Angry, and scared we arrived at Mass General Hospital ER as advised where we were immediately triaged and taken back to a room for further testing, and assessments. Additional lab work was done, imaging studies were ordered STAT, they covered literally everything from head to toe. Just as my husband was dozing off, the ER doctor came back in to advise us that his symptoms were likely related to a Right lower lob pneumonia they had identified on exam. They would start him on some antibiotics and get him home within 24 hrs.
Less thanfive minutes later the ER doctor returned, this time with a little less pep inhis step and said, Mr. Perry, I’m sorry, I spoke too soon. Our testing showsyou have a blood cancer called Leukemia, we are going to admit you to ouroncology floor where you will be assigned to an oncology team who will explainthis in more detail, and likely do further testing, etc.
Leukemia? How could this be? This is a man who defied all odds, coming back from a fall from over 220 feet less than a year and a half ago. There must be a mistake! Our lives were just returning to some normalcy. How will I tell our girls? How will I watch the man I love suffer more than he already has? Where will I find the strength? As I looked beside me, the answer was already there-my sister Lisa.
You see, sadly her beautiful son Aidan was diagnosed with Stage 4 Wilm’s tumor (Kidney cancer) that had spread to his lungs at the age of 3. Ironically, I was the one sitting right next to her as she learned of her sons unfathomable diagnosis. I was her pillar of strength and now she would be mine.
My husbandhad every complication you can imagine. In fact, we were told by his oncologyteam, once stable, that he was the sickest patient on the oncology floor andthey were unsure if he would even survive.
Official bonemarrow studies confirmed a High Risk APL diagnosis, with the FLT3 mutation. HisWBC on admission was close to 30, with a platelet count of 7. He was immediately started on intense chemotherapy as an inpatient where he would spend the next 30 days.
They covered him for every bacteria possible but were losing hope when antibiotics were not resolving his pneumonia. During this time, he required maximum oxygen support due to DIC a major life-threatening bleeding complication associated with APL specifically. He came very close to being placed on a ventilator, and I was prepared by the oncology team for the worst.
Althoughplacing him on a ventilator would help his body and lungs rest and heal, thiswas still a last resort. A bronchoscopy could not be done due to the risk ofbleeding, once again as a result of DIC. So, we waited, and in time hisbreathing improved requiring less oxygen every day. We were finally moving inthe right direction. Unfortunately, during this time, DIC also causedhemorrhaging behind his eyes, resulting in acute vision loss which laterresolved when his platelets normalized. He will now be followed regularly byophthalmology to monitor for any lasting side effects.
Finally,after approximately 14 days, he began to turn the corner. While inpatient hecontinued to receive blood transfusions as necessary, platelets, packed cells,antibiotics, antifungals, as well as oral and IV infusions of chemotherapy. Hetolerated these medications fairly well complaining of headaches, nausea,decreased appetite and intermittent diarrhea. His counts seemed to take alittle bit longer to recover, but they did and that’s all that really matters.
A bonemarrow biopsy was done prior to discharge that revealed thankfully he was inremission. We would continue outpatient chemotherapy for the next 6 months inhopes of achieving molecular remission. His consolidation regimen would includeATRA, and IV Arsenic infusions as instructed. He was prescribed additionalsupplements of Potassium and Magnesium to take while completing this regimen oftherapy as well.
Outside of extreme fatigue, headaches, and severely dry, itchy skin, he was able to maintain a healthy weight and go out socially from time to time. Due to the nature of this illness and his exposure working with the public, it was recommended he not return to work while in active treatment. Unfortunately, due to extensive surgeries from his previous accident he had no sick time or disability time available to cover the time he would need to be out of work. We worked with the hospitals resource department to see what, if anything they could do to help our family financially during this time.
Unfortunately, we were told there weren’t a lot of resources available for Leukemia patients. This was REALLY difficult to hear. Thankfully through the support of our amazing family and friends we were able to get through this time with their support emotionally and financially. But what if we didn’t have this support? We were lucky, but what if we weren’t?
As if thestress of worrying about saving my husbands life was not difficult enough,having to worry about the roof over our heads, supporting our car payments toget to and from treatments, paying for gas, daily parking, and putting food onour table would have simply been impossible. This has been really difficult to manageand our fight with creditors, etc. remains ongoing.
Our childrenhave been impacted tremendously by their dads illness. After almost losingtheir dad once, their hearts already had a lot of healing to do. They are so sofragile. As we get closer to the end ofhis treatment, they are becoming more confident their dad is going to be ok butnonetheless, it has been a long, hard, emotional road for all of us, butespecially for our 3 beautiful daughters. We take absolutely nothing for grantedand realize how lucky we are to have one more day together.
It is my goal, once I can finally see the light at the end of all this, to find a way to raise more awareness, and funding for this seemingly under-funded disease.
I MADE A SPLIT-SECOND DECISION TO MAKE THIS A POSITIVE JOURNEY

September 19, 2018 – So You’ve Got Acute Blood Cancer…Join the Club!!!
BY: RICK GAGNON (dakota19@gmail.com)
At 1:00pm on Saturday, March 11, 2017, I was diagnosed with Non-Philadelphia B-Cell Acute Lymphoblastic Leukemia (ALL).
My name is Rick Gagnon. I am a 57 year old father of 2 adult children, Jocelyne and Jeremy and grandfather to my beautiful grand-daughter, Olivia. I have been, and continue to be supported by my loving wife, my ‘rock’ of 32 years, Tracey.
On that Saturday morning, as I was preparing to shower, I noticed a very large bruise just above my left hip. I went to show my wife and she noticed several other bruises all over my body. Tracey was concerned about internal bleeding so we immediately made our way to the Emergency Department at the Juravinski hospital in Hamilton, Ontario.
When I indicated my symptoms to the triage attendant, I was immediately moved to Intermediate care and put through a battery of blood tests, x-rays and ultrasounds. Less than three hours later, the attending Hematology Oncologist told us I had Leukemia. At first, we were in complete shock. After a few minutes to absorb this devastating diagnosis, we took a deep breath and then an exclamation, by me, of “Ok, let’s get this party started.” As stunning as the news was, I made a split-second decision to make this a positive journey which garnered looks of amazement from the doctor and the support staff.
I was admitted immediately and my case was handed over to Dr. Brian Leber, Professor, Medicine, Hematology and Thromboembolism at Hamilton Health Sciences. As a clinical hematologist, Dr. Leber’s clinical focus revolves around the pathophysiology of leukemia.
On Monday morning, Dr. Leber met with my family and I to share with us my complete diagnosis and the treatment protocol that would become my ‘two-year adventure’. In his summary of my diagnosis he noted that my timing was impeccable. Had I come in to the hospital two days earlier, there was a good chance I may have been misdiagnosed. Had I come into the hospital two days later, I likely would have died from a massive brain bleed.
And so, my adventure began that Monday evening with my first chemo treatment.
It’s now been just over 16 months since my journey began. We have encountered a lot of ups and downs, we’ve cried, we’ve laughed, we learned a lot about blood cancers and we’ve met some amazing people both professionally and personally.
During my recovery, I can often be found at the Juravinski hospital visiting with blood cancer patients who don’t often get visitors. Support, a positive attitude and faith are a huge part of our treatment. I do this to make it a less traumatic experience for them. I often leave them a copy of a devotional book that has been a staple of my daily faith.
I also spend time peddling PICC line sleeves that resemble a sleeve tattoo. I sell them for $10 with all proceeds going to cancer research. People love them and they are a great alternative to socks or that mesh sleeve they give you in hospital.
I have been blessed during my journey. Between my family, my friends and prayer, my journey has been very humbling. To that end, at my July 31st weekly chemo day visit, I was told that I was officially in remission. That was a huge weight lifted from shoulders. Each day I wake up, I am a survivor and that is all the motivation I need to get through my journey. I take everything one day at a time. I make the most of each day and I do my best to share my story with others in an attempt to educate them about blood cancers.
So, my journey continues. Without any more delays, my ‘bell ringing’ day should be June 25th, 2019.
Thank you for joining in my journey.
I TOOK PAIN MEDS, ICED THE SPOTS THAT HURT, AND CONTINUED WAITING FOR THE PAIN TO GO AWAY

July 31, 2018 – So You’ve Got Acute Blood Cancer…Join the Club!!!
BY: ALEXA PICKENS (pickens@ualberta.ca)
I was 19 years old when I was diagnosed with cancer. I was in my second year of University, and overall, I was exceedingly healthy at the time. I worked out regularly, focused on my school work, ate healthy and I didn’t smoke or drink. The diagnosis came as a complete shock, and the life-threatening complications that I endured during treatment were just as incomprehensible.
It all started in October 2013, when I woke up in the middle of the night with the most excruciating pain I had ever felt. I remember crying in agony, popping pain meds like they were candy and laying on the floor trying to get back to sleep so I could be rested enough for my midterm exam the next morning. The pain subsided enough for me to catch a couple more hours of sleep, but the pain would not let up for a week. This viscous cycle continued for 4 months. I was in tears from the pain and lack of sleep. Going to school, working out, and working were next to impossible, but having been an athlete most of my life, I took pain meds, iced the spots that hurt, and continued waiting for the pain to go away, all while I tried to live my life as normally as possible.
Finally in February 2014, I went and saw my doctor, no longer able to handle the pain and exhaustion. The bone scan I did revealed that I had a compressed facture on my L5, and after further investigation with an MRI, it was determined that a tumor had caused the fracture. There were also more tumors spread along my spine, neck, pelvis, ribs and sternum. I was given high doses of steroids, morphine and valium while doctors and pathologists tried to figure out what kind of cancer I had and over the next 2 months would be poked and prodded more times than I can count or remember. First doctors thought I had Lymphoma, then Multiple Myeloma, then Ewing’s Sarcoma. The results of bone marrow biopsies and blood work always came back either inconclusive or normal. The only thing doctors were sure of was that I did, in fact, have cancer. They eventually determined that it was a form of leukemia but were unsure if it was Acute Promyelocytic Leukemia (APL) or Acute Myelocytic Leukemia (AML), and had no definitive way of determining which one it was.
I was about to be referred to the Mayo Clinic in the States when I got the call on April 22, 2014. I was finally diagnosed with APL after 2 very long and uncertain months. I went to the hospital that night, and the next morning I began my first dose of ATRA, followed by Idarubicin, and then Arsenic + ATRA. Treatment was going really well. I was almost bored as I was not feeling any side effects from the chemo. I was running out of shows and movies to watch while I lay in my hospital bed.
Unfortunately, about 11 days into treatment, the boredom was replaced with chaos and I began my first bout of complications. This would continue for the next 3 months and almost take my life on more than one occasion. My heart needed to be restarted twice as it was beating at an alarming rate, I developed differentiation syndrome –extreme swelling of the body- which caused my small intestine to perforate, and bleed profusely for weeks. During this time, I developed a blood clot close to my heart due to the PICC line that was inserted in my arm, and then became septic due to the tearing in my bowels. The sepsis caused bacterial meningitis. Since this had gone undiagnosed for so long, I needed emergency surgery and was put on life support as I was comatose and showed little to no cognitive function. My family was told to say their goodbyes and there wasn’t anything more they could do for me. At this time my family sent my file over to a family friend who works for the CDC in Winnipeg. He discovered a procedure that involved injecting vancomycin through the temporary shunt directly into my brain. This procedure has only been done a handful of times successfully in the States, but has never been done in Canada. When my family brought this information back to the ICU doctor, he explained the risks to my family. He told my family that this injection could do 1 of 3 things: it would do nothing, it would kill me, or if it worked, I would be left with severe cognitive and physical impairments and most likely need to live in an assisted living facility of some kind. My family decided to go along with the injection despite the risks. Several hours later they were told to come back and say goodbye, as the injection didn’t seem to have worked. Fortunately, the next day my stats began to improve, and I was beginning to make a miraculous recovery. I ended up developing hydrocephalus because of the infection in my brain, and so I was rushed into surgery for a second time where the surgeon inserted a permanent shunt into my brain to help with the inflammation and fluid build-up.
During these months, I had spent 41 days in and out of ICU in critical condition and lost a staggering 50lbs. I was 140lbs when I started treatment, and dropped down to 90lbs. I suffered severe muscle atrophy in my arms and legs; so much so doctors told my family I would never walk without a mobility aid of some kind. I don’t remember most of what happened to me as I was in and out of a comatose state and given high doses of fentanyl, dilaudid, and morphine during these months.
I was eventually able to leave the hospital and resume my treatment as an outpatient. I needed to learn to walk again and gain my strength, so after chemo, my nights consisted of physiotherapy, occupational therapy, and recreational therapy to help me regain function in my brain and muscles. I was hopeful it would help reverse some of the deficits I had developed. My family was not sure if I would ever regain full cognitive or physical function again, there was still so much uncertainty about what my future would look like… It was exhausting, and there were so many times I wanted to give up. I had developed a severe skin reaction as a result of the treatment and had painful blisters and rashes throughout my entire body. Physio exercises, let alone moving in general, was extremely difficult. I was told I was in remission on October 09, 2014 and finally finished my IV treatment January 23, 2015, resuming with the maintenance round up until November 20, 2016. During this time, I had returned to my studies, and eventually transferred universities to pursue recreational therapy. School became a great distraction for me and gave me a bit of the normality back that I had been craving so much.
A week after I finished my maintenance round, I experienced severe pain in my left hip and began limping quite a bit. I, of course, ignored the pain as it was far too familiar from the pain that I had felt from before; I didn’t want to believe that my start to a new life was going to consist of more pain and more doctors. February 10, 2017 I was diagnosed with Avascular Necrosis in both of my hips because of being on high doses of corticosteroids and treatment. I had a bilateral hip decompression surgery on May 15, 2017 in hopes of treating this condition. Unfortunately, it did not work, and I would require a full replacement of my left hip.
Being diagnosed with cancer at 19, put on life support at 20, going through chemo treatment at 21 and 22, having hip surgery at 23, and a hip replacement at 24, I have struggled with feeling like my 20s have slowly slipped away. This is supposed to be a time about finding yourself as a person, getting your undergraduate degree and maybe your masters, and starting a career. I am going to get my undergraduate degree, and I will eventually get to where I want to be in life, just not the way that I once thought I would. Trying to live a normal life with chronic pain and dealing with medical issues has not been easy, but it has taught me how fortunate I am, and how resilient I am. It has shown me that no matter what life throws at me, I will be able to get through it. There is a purpose for me. These past 4 years of my young life have taught me so much, and I am forever grateful for that. It’s so easy to look at the negatives in our lives, but when we take the time to see the good, to see the positives, we realize how lucky we are and how strong we are, and most importantly we learn to appreciate the little things in life and those who have stuck by when things went a little south.
AS SOON AS THE DOCTOR ASKED ME HOW OLD MY KIDS WERE, I KNEW I WAS IN TROUBLE

July 15, 2018 – So You’ve Got Acute Blood Cancer…Join the Club!!!
BY: MICHELLE BURLEIGH
I grew up in a household that struggled financially and the focus always seemed to be getting through a day rather than living a day. I’ve never been the type of person to accept anything less than exactly what I want. Coupled with an intense drive for financial security, this led me to spend the majority of my adult life believing that success is associated with career development, financial gains and material things. Later, my daughters future success also became part of that focus.
I graduated high school in 1998 and went straight to work. In 2001, I fell into the financial industry when I landed a job with a major credit card company in Vancouver, British Columbia. As it turns out, I really enjoyed learning about the financial industry and helping people. Over the last 17 years, I have worked tirelessly to drive my career forward, sometimes to the point of crashing and suffering physical illness and mental exhaustion. All the while, focusing very little attention on nutrition and wellness. At times in my life I’ve decided to lose weight (let’s be real, every summer for a new Caribana costume and tropical vacations), usually it was done by liquid diet, starvation and insane working out. Wellness was limited to getting on a plane to party for a week (Caribbean partying? No regrets there!!!).
The birth of my first daughter, Victoria, really sparked my interest to learn about having a proper nutritious diet. Growing up on processed foods and sugar, like everyone else in the 80’s, has unfortunately led to battling brutal eating habits. Quite frankly, has very likely contributed to me being right here writing this story. I have spent the last 6 years struggling to make healthy choices and ensure she, and then they, are raised having a healthy relationship with food. To be honest, Victoria has an iron clad will and is as stubborn as her mother (my mantra is, ‘It will do her good in the long run’…usually accompanied by wine). Isabelle is an awesome eater. Victoria and I certainly have our food struggles now but if at 6 years old she feels like she’s rebelling from the cooked vegetables I put on the table for raw ones in the fridge, we both win every time.
I started feeling generally unwell toward the end of November 2017. I started having headaches that were impacting my vision. The pain wasn’t unbearable but I couldn’t see which was scary. They also seemed to come on with physical activity; cooking, grocery shopping, housework. I didn’t think much of them because it was November and still hot outside. I figured it was just related to the unusual weather. After a workout at the gym, a muscle in my hip locked for a number of days. I visited my doctor who prescribed a pain reliever called Meloxicam. Within 24 hours, I started bruising for no apparent reason. The following day, the bruising became worse. Some of them were small and irregular shapes and colors. Some were large and dark and puffy. I also noticed that I was incredibly fatigued. In fact, I couldn’t even finish preparing dinner for my family that night. I was too tired, and one of those strange headaches was taking hold. I had also broken out in coldsores on my mouth like I’d never had before and they weren’t healing. The day before I was diagnosed, I noticed blood vessels bursting on my arms. I had also started my menstrual period and the amount of blood was unlike anything I had every experienced before. I had called my doctors office twice during the course of these 3 days prior to diagnosis and was told what I was experiencing was likely not medication related and I should call my pharmacist for more information about the medications (have I mentioned bruising, breaking blood vessels and excessive bleeding and tell tales signs of leukemia?). I was even scolded by my doctors office manager who didn’t like my tone. Side note, I have a new doctor now. I visited the emergency room the next morning. In retrospect, I should have known sooner that there was something seriously wrong. But as a busy mom and career woman who was in the process of preparing for Christmas parties, hosting Christmas dinner and just living the daily grind, I did not have time to feel sick. So, I ignored it and kept going.
I spent 5 hours at the hospital the morning after the bleeding started, after having to argue with the triage nurse to even see a doctor. I guess I didn’t look sick enough? They took bloodwork which revealed some odd results and so they sent my blood to another hospital for further assessment. The doctor did mention that my platelet count was low and it could be anything from my spleen eating up platelets to, worst case scenario, cancer. It was said so non-shalantly. Ironically, I clearly remember thinking, ‘I hope it’s not my spleen. I don’t want to have surgery!’. I was more worried about scarring and cancer didn’t even register as a possibility.
I’ll never forget the doctor coming into the room with the diagnosis. She asked me how old my kids were and I knew I was in trouble. I didn’t answer her question and instead asked her one in return, ‘Is it worse case scenario?’. She said, ‘It’s never easy to tell anyone this. You have leukemia’. My first thought was, ‘People don’t come back from this. I’m going to die’.
It was terrifying and devastating. As a seemingly healthy woman, raising young daughters and nurturing a thriving career, I thought, ‘I’m not done here yet’.
My mother and I already had plans to spend that afternoon together so when she arrived at the hospital, I told her the news. I immediately texted my boyfriend to leave work immediately and come to the hospital. He was in the hospital room with me within an hour. I told him in person in the hospital. I felt sorry for my mom. Like I needed to protect her from what was coming. And I felt shame when I told my partner. I felt that we are too young to be dealing with this. We should be happy and growing together and thriving together. Instead, I knew I would have to rely on him to help me through whatever was coming and he may even have to face my death only months after losing his father. I felt guilty. As a mother, I immediately felt helpless and inadequate. Like I had failed my kids.
The immediate 80 minute drive to Juravinski Hospital in Hamilton, Ontario, where I would be admitted for treatment, is the time I used to call my father, brother and best friends. Two days later, the hematology team confirmed that I had Acute Promyelotic Leukemia. When my oncologist visited me in my room to share the news he was very clear and concise in his explanation of what we were dealing with, and what was in store in the coming days, months and years. He told me that APL is a subtype of Acute Myelotic Leukemia (AML) and one of the most rare forms of leukemia. He also told me there was good news and bad news. The good news was, it is the most curable form of leukemia and the prognosis was 90% full recovery. The caveated was, I had to make it through the first 10 days of treatment. He also followed up that statement by assuring me that I was young and healthy and my chances were good. And finally, he revealed that the disease was so far advanced at the time I was admitted that had I not visited the hospital, I would likely have experienced an internal bleed that would have killed me within 24 hours.
It’s incredible how the human brain processes this kind of news…or maybe just doesn’t right away. There was no time to digest this information, there was no discussion about options. I was dying and I had to trust these people to stop that from happening.
I don’t think I felt much at the time the doctor shared this information. I did not have time to feel anything. I was headed into the fight of my life and my energy needed to be 100% focused on the fight. I focused on things like how much my daughters need me. I focused on the home renovations my partner and I wanted to do. I focused on all the things we wanted to do with our family, like getting married and taking our kids on a Disney cruise.
The first time I was really afraid after the initial diagnosis was the night my heart rate dropped. I had already received my first dose of a chemotherapy called Idarubicin and nicknamed ‘The Red Devil’ and it turns out it is very appropriately named. My heart rate dropped to 38 beats per minute and stayed between 40 – 50 beats per minute for a week and a half.
I did a great job of ignoring the fear during the day but when I laid my head on my pillow at night and couldn’t feel my heart beating in my chest, the fear took hold. It was the most lonely and helpless feeling in the world. I started writing people. In particular, people I hadn’t seen for a long time and thought should know I might not be around much longer and people who I had insights about that I wanted to share before it was too late. For example, the owner of the nail salon that I had started visiting a year earlier. She is a kind, compassionate and brave human being and I needed to tell her that (go see her at Pink Nails & Beauty in Georgetown, Ontario!!!). I spent countless hours looking at pictures and videos of my family, reminding myself why my heart could not stop. My family needed me.
I spent 22 days in the hospital receiving red blood cells, platelets, cryoprecipitate (my blood wasn’t able to clot on it’s own), antibiotics, chemotherapy, x-rays, ultrasounds…the list goes on. I finished the first phase of treatment in mid-January 2018 and at the end of the month received the results of my second bone marrow biopsy. I was in remission, and the cancer was undetectable. I don’t think I’ve ever felt so relieved about anything in my life as I was when I got that phone call.
After 4 more months of IV treatment almost daily at Juravinski, I started the final phase of treatment. This is the longest and least climactic phase of treatment as the immediate danger has passed and we are now working towards maintaining remission. As it turns out, I have a genetic mutation called FLT3 which puts me in the high risk category. Meaning I will take oral chemotherapy for a total of 2 years following IV treatment. I’m not exactly sure what the long term looks like for me. What I know is, emotionally, this is the hardest phase to deal with. Not only have all of the emotions I didn’t allow myself to feel over the last few months whack me like a Louisville Slugger, I also have to come to terms with the reality of my new normal. The world can be a scary place after treatment and learning how to live life to the fullest and manage the new threats like, sun sensitivity, long/short term medication side effects and post-treatment trauma is no small feat.
I have spent my whole life planning for the future, working hard and spending very little time in the present. While planning and working hard for what you want is important, NO ONE is guaranteed tomorrow. While, I wouldn’t wish this on anyone, I can honestly say there is a silver lining. I’ve come to the realization that when I am laying on my actual death bed (hopefully when I’ve had many many years of dragging Marvin out on crazy adventures), I won’t be thinking to myself, ‘Man, I really wish I had moved that light fixture in the ensuite bathroom!’. It’s the time we spent together, living life, having fun, appreciating our family and watching our kids grow. That’s what I want to remember on my dying day.